Nadira Danielle Gray was scared.
She’d just turned 40, and her family medicine doctor told her it was time to start getting mammograms. But to Gray, even the idea of a cancer screening was too much. The two most beloved women in her life had died of cancer: her mother of brain cancer, her grandmother of lung cancer. Her aunt was battling breast cancer.
“You got this wrong,” she told her doctor. “I’m too young for this.” But her physician explained that guidelines had changed and, in fact, 40 is now the recommended starting age for breast imaging for most women.
Still, she says, “The C-word just terrified me.”
Gray shared her concerns with her trusted pastor, Terrilynn Donnell, who leads The Church of Christian Compassion in Cobbs Creek. Donnell was adamant that Gray get tested. “There’s nothing wrong with you, but you always want to make sure that if anything is going on, you catch it early,” Gray says Donnell advised her. “She really encouraged me to do it.”
Cancer screenings come to Cobbs Creek
As timing would have it, the church and its community center, the Community of Compassion CDC, were just about to host a neighborhood health fair — and no ordinary health fair. Rather than simply providing information and, say, branded stress balls, as health fairs often do, this event in partnership with Penn Medicine and Siemens Healthineers would be a high-tech affair.
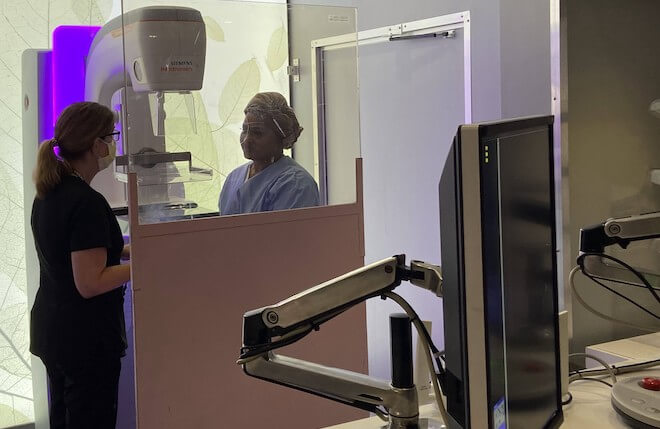
The City agreed to block off one block at the intersection of Cedar Avenue and 61st Street, where the church and community center are located, to set up screening stations for lung, colon, and prostate cancer, as well as other chronic diseases. Around the corner, in the parking lot of the Fresh Grocer, Siemens Healthineers set up “Mammo Mandy,” its mobile mammogram van with the most advanced breast screening technology on the market. Also on hand were volunteers from Penn Medicine to help assign attendees to a Penn physician for follow-up care, and to help folks who were un- or under-insured get signed up for healthcare coverage. A church van shuttled women to and from the church to the Fresh Grocer every 20 minutes.
“Because it was a partnership with my church, I knew that I could trust it. Anything that partners with my church, my place of worship, makes me more comfortable and more willing to take part in it,” Gray says. Plus, she says, it was too convenient not to go. “I didn’t have to worry about transportation — it was literally being brought right to me.”
Gray’s experience is more than a feel-good anecdote. This kind of creative collaboration is exemplary of a way Philly is working to change the disparities in healthcare for women — who are more likely to have their symptoms doubted; more likely to prioritize the health of those they care for over their own health; have higher rates of obesity, high blood pressure, and high cholesterol; are at a higher risk for heart disease; and are also, as a function of their sex at birth, at a higher risk for complications related to menstruation, pregnancy, delivery, menopause, and so on.
This kind of creative collaboration is exemplary of a way Philly is working to change the disparities in healthcare for women.
Healthcare disparities are even more pronounced for women of color, because of what many health experts refer to as social determinants of health: housing, food insecurity, education, economic status, neighborhood and environment, and access to high-quality healthcare. These factors date back to centuries of institutionalized racism, and the related barriers to care that have sprung up as a result: Mistrust of the medical community. Childcare and transportation costs and the job flexibility required to get timely care. Lack of adequate or affordable health insurance. And so on.
When it comes to breast cancer, this has deadly consequences. According to the American Cancer Society, Black women have a 4 percent lower incidence rate of breast cancer than White women, but a 40 percent higher breast cancer death rate. Black women are more prone to a certain type of aggressive cancer. But, according to Breast Cancer Research Fund, Black adults have higher death rates from most cancer types because they are more likely than White people to be diagnosed with an advanced disease — for all of the reasons above, they are not getting mammograms as early, or as regularly, as White women.
That’s what makes the Penn/Siemens Healthineers/Community of Compassion collaboration so important. The health fair eliminated many of the barriers between Philadelphians of color and the healthcare system, by literally bringing the care to patients where they live, relying on trusted messengers, and taking on the costs of full-service care, from providing insurance navigators to assigning physicians to follow up with results and after-care.
“When we partner with the community, we get an idea of how to better serve individuals, what the people feel they really need — not what we think that they need,” says Penn Medicine’s Linda White Nunes, MD, MPH, vice chair for inclusion, diversity, and equity for the department of radiology.
The legacy of Covid
Penn Medicine first partnered with The Church of Christian Compassion during the pandemic to bring the community, which is largely Black and historically medically underserved, Covid vaccines and support food distributions. The event was so successful that, when Nunes felt a pull to do more community events, the church was the first group to come to mind. In 2021 she reached out to Pastor Donnell to gauge the community’s interest in an educational health fair.
But what Donnell and her team wanted was more than information — they wanted start-to-finish care. Nunes got to work with her colleagues at Penn Medicine; simultaneously, Siemens Healthineers, whose Diagnostic Imaging U.S. Headquarters are in Malvern, happened to reach out to Penn to find out how they could be more involved with community outreach.
With these three main pillars — healthcare, industry, and community — coming together, the partners spent the next six-plus months working on planning and outreach. Markeeda McClean, Donnell’s Executive Assistant, went to all of the schools in the neighborhood, asking teachers to share information about the fair with their parent list-servs. Congregants shared rousing testimonies about their breast cancer journeys during services. Nunes tapped colleagues from across the entire health system, from finance and billing to oncology and radiology and marketing.

With such coordinated efforts, the results were far greater than what anyone originally envisioned: a full-day health fair in June 2022 following a Sunday church service. The event provided screenings for the four most common cancers. Insurance navigators were onsite to help folks who are un- or under-insured find coverage. Everyone was assigned a Penn physician who’d be the point person for follow-up care (with the option, but no obligation, to stick with Penn for care). Attendees were given a “health fair passport” with all stations noted on it; those who visited every station were entered to win a raffle for prizes like iPads and AirPods. On top of the day-long multi-specialty fair, there were an additional two weeks of mammogram screenings onsite in the community.
The event was so popular that it was held again in June 2023, when Gray attended. Another one is scheduled for June 2024.
“It goes to show that by putting people in the same room, with the same focus, how much could really be accomplished,” Nunes says. “Each group makes the other better.”
A replicable blueprint
As the data from the fair came in, what Nunes and her colleagues found was staggering. “For the June 2022 fair [the most recent one for which all data is available], our cancer detection rate was about 2 to 3 times the expected rate,” she says. “That says that we’re reaching people who don’t ordinarily get screened, and that’s what we were really setting out to do.”
More specifically: 181 women received mammograms, and 21 (12 percent) had abnormal results. (Another 32 attendees got prostate-specific antigen tests, 9 got fecal immunochemical tests, and 10 got assessments of eligibility for low-dose chest computed tomography.) Data is still coming in for the 2023 fair, but Nunes reports that more than 300 women received mammograms — an increase of 100-plus from the year prior.
Abby Weldon, senior director of women’s health at Siemens Healthineers, says that her phone has been ringing nonstop since the success of the Penn program, whose findings were published just this month in the journal Academic Radiology. But it takes an intense level of investment — of money, resources, and determination — to pull it off.
“When we partner with the community, we get an idea of how to better serve individuals, what the people feel they really need — not what we think that they need.” — Linda White Nunes, Penn Medicine department of radiology
“It’s a really heavy lift on a healthcare provider [like Penn’s] part,” she says. Siemens Healthineers was able to provide the mammogram machine because Penn agreed not to take any reimbursement for these screening exams, and they agreed to take on navigation of aftercare as well — notifying people of their results, and getting anyone who required follow-up testing in to see a Penn clinician. “Not every facility [is] able to do that,” Weldon says. “Not every facility has a Penn Medicine behind it.”
And the community partnership, Weldon says, is what unlocked the full potential of the program. “The proximity and the trust is the most important part,” she says.
For Gray, the experience was nothing like the nightmare she dreaded. For one thing, the mammogram was far less uncomfortable than she expected, a credit to Siemens Healthineers’ technology, which uses a proprietary algorithm to make sure mammograms use only — and no more than — the precise amount of breast compression to get the clearest image possible. It helped, too, that the friendly technicians, a group whose diversity reflected that of the community, patiently explained every step of the process to Gray.
But the best part for Gray? Getting her negative result. “With cancer running rampant in my family, going to the screening and finding out that there is nothing wrong with me has reassured me that their story doesn’t have to be my story,” she says.
“I always heard the saying What you don’t know can’t hurt you, but that is a lie. What you don’t know can hurt you and can devastate your family and your life. So the sooner you find out, your prognosis will be better than if you just waited because you were afraid. Being afraid can end your life — being bold and brave can save it.”
This piece is part of a year-long editorial series looking at innovations to address inequities in women’s healthcare, sponsored by Independence Blue Cross.
![]()
![]() MORE ON HEALTHCARE FROM THE CITIZEN
MORE ON HEALTHCARE FROM THE CITIZEN



