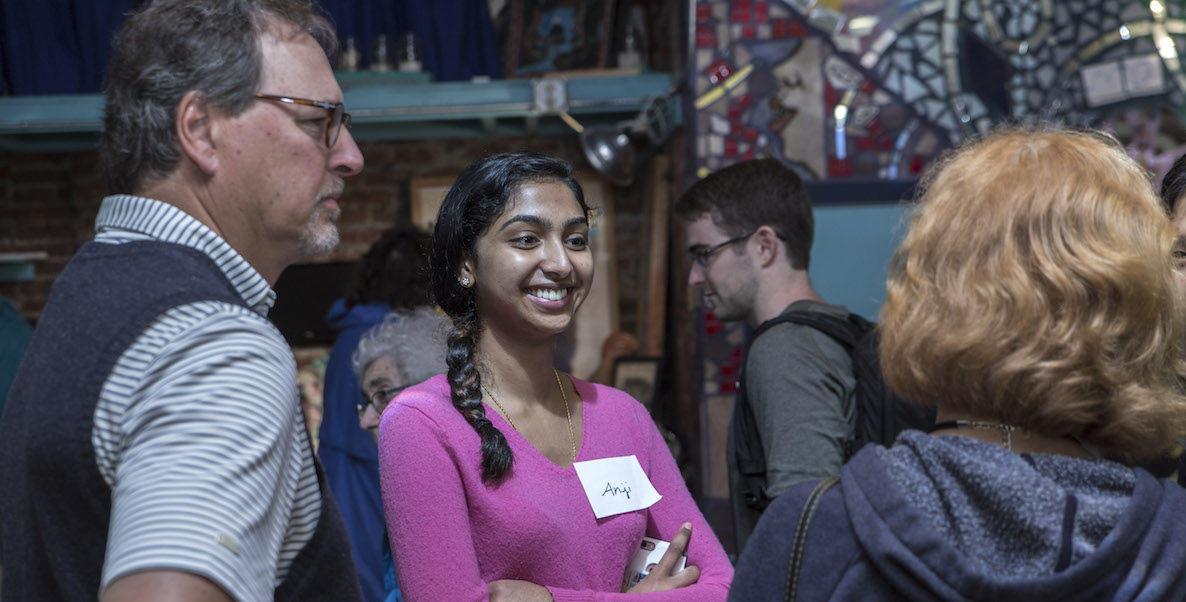It was at an unexpected venue for medical school training that Jeff Lee, a young Thomas Jefferson University student, took away one of his most important lessons last year. At South Street’s Magic Gardens, Lee was admiring mosaics with a couple he had just met through an elective, ARTZ@Jefferson. Mary Anne, suffering from early onset dementia, stopped before a section of wall and said it reminded her of a frog. Then she launched into a story, a happy memory of chasing frogs when she was a child.
For the first year medical student, new to Philly and to medicine, the moment was mind-opening. Lee saw the patient light up, felt who she was—beyond the dementia—and genuinely connected to her, and what she was experiencing. It was something he would not soon forget—he went on to become friends with Mary Anne and her husband—and that he will, hopefully, come back to again and again in his years of learning and practicing medicine.
The Magic Garden visit was part of a larger course for first and second-year medical students with one specific intention: Teaching empathy to those who will be encountering sick and often distraught people for the rest of their lives. The program, which last week was awarded a $300,000 Pew Center for Arts & Heritage grant, uses museum visits as a way to connect healthcare students to patients with dementia and their caregivers. The hope is that the conversations that spring from the art will lead to conversations about life as a person suffering from dementia, or caring for someone with dementia—and will also allow patients to better understand the young people who may one day become their doctors.
Studies have shown that the patients of doctors who have high levels of empathy fare significantly better, including those with diabetes and the common cold. “When there’s an empathetic relationship between doctors and patients, there’s more trust,” says Mohammadreza Hojat, a Jefferson professor who has long studied empathy.
“People with dementia feel marginalized in health care,” says Megan Voeller, director of humanities at Jefferson. “And students are trying to figure out the type of healthcare provider they want to be. That’s a challenging, difficult process. It behooves society to build more bridges between these groups of people.”
There are more than just feel-good reasons for teaching empathy to medical students. Doctors experience professional burnout at a higher rate than other American workers, partly because over time, they start to feel disconnected from what they’re doing, to lose the meaning of their work, the reason they started practicing medicine to begin with. Voeller says connecting more meaningfully with their patients, and with each other, has shown to reduce this effect.
And studies have shown that the patients of doctors who have high levels of empathy fare significantly better, including those with diabetes and the common cold. “When there’s an empathetic relationship between doctors and patients, there’s more trust,” says Mohammadreza Hojat, a Jefferson professor who has long studied empathy. “When there’s more trust, all the constraints will be diminished. The person will tell more of the story, which will lead to a more accurate diagnosis. And the patient is more likely to follow the physician’s advice. Better diagnosis and more compliance result in better patient outcomes.”

Hojat’s work dates back about 17 years, to when medical educators first started talking about the importance of empathy in caring for patients. At the time, there was no clear definition of empathy, and the role it played in medicine, so Hojat created a Jefferson Scale of Empathy assessment, which is now used in medical schools around the country and has been translated into 55 languages.
Hojat’s research found that by the time students were in their third year—starting their clinical training, seeing actual patients—their empathy had significantly diminished. (Voeller says this may be partly a matter of how they learn in their first two years of coursework, studying the human body as made up of anatomy and physiology, but not so much emotions.) And medical schools have started to pay more attention, targeting young students, before they have a chance to lose what often led them to medicine in the first place—helping others.
Jefferson is a leader in combining the study of medicine with an active focus on empathy—starting with its admissions process, which looks for students who exhibit some emotional intelligence. Under President and CEO Steve Klasko, the university has also expanded its use of arts programs to encourage close listening or observation—an abstract way to nourish empathy skills. Klasko, in a TEDx talk in 2014 describes how this plays out at Jefferson (see around the 7:45 minute mark):
ARTZ@Jefferson takes a more direct approach: Students sign up knowing that it is a lesson in empathy. It will be offered next year to 15 to 20 students per semester, a number limited by how many dementia patients the program is able to recruit.
ARTZ@Jefferson is an offshoot of ARTZ Philadelphia, a four-year-old nonprofit started by art historian/curator Susan Shifrin, who uses visits to art museums to foster conversation and community among patients with dementia and their caretakers. Shifrin—whose mother has had dementia for 16 years—first started working with dementia patients when she was an art educator at Ursinus College’s art museum.
“What I saw at the galleries was sort of stunning,” Shifrin recalls. “I got to know some of these people in their own setting, and they didn’t talk much. They got to the gallery and they came to life. Focusing on art, on something outside of themselves, on something everyone else is focusing on, allows people with dementia to shed some of the constraints the illness can impose on them.”
“Now what students are going to see when they see someone with a chronic illness—not just dementia—is a person with a life, a history, extraordinary experiences. They get the idea that patients are people first, and then patients,” says Shifrin.
Shortly after she started ARTZ Philly, Shifrin offered a truncated version of ARTZ@Jeff to Drexel University medical students, with Drexel professor Florence Gelo. Last year, Shifrin and Gelo were invited to bring their program to Jefferson.
Next year, ARTZ@Jefferson will consist of 10 sessions over the course of a semester. First the students, patients and caregivers will meet at a museum and then participate in a led discussion about what they saw and what it means. At the end of that visit, students are paired with patients/caregivers for the remainder of the course. The next few sessions will alternate between collective art gatherings—including at the Barnes Foundation and the Woodmere Museum—and student-only meetings, in which Shifrin and Gelo will help the students unpack what they’ve learned, and how to grow their relationships with their mentors. The last part of the course is a new addition. Working with Theater of Witness, a group that brings together people from different sides of an issue to create theater, the students and their patient/caregiver mentors will work to script a play, that they will then perform.
“Students have told us they realize now that it was all too easy to look at someone with dementia as just a ‘dementia patient,’” Shifrin says. “Now what they’re going to see when they see someone with a chronic illness—not just dementia—is a person with a life, a history, extraordinary experiences. They get the idea that patients are people first, and then patients.”
As part of the Pew grant, Shifrin plans to hire an ethnographer to catalogue the experience, and the stories that come out of the program. And Jefferson plans to give students the empathy assessment before and after the semester, to gauge its effects—though Voeller acknowledges that with such a small student population to start with, the survey may not be conclusive, and the effects may not be long-term.
Still, this is, clearly, a different way to approach the teaching of new doctors. The ![]() programs at Jefferson address what Hojat calls the “art” of medicine, something he says the medical profession spends too little time on. Most of medical training is about science—physiology, anatomy, pharmacology. Lessons in empathy and personal attention, though they are now included in healthcare education, often end with the close of a humanities elective. But empathy needs to be reinforced, Hojat says; it fades over time. And he argues that it should be part of continuing education for healthcare professionals throughout their career.
programs at Jefferson address what Hojat calls the “art” of medicine, something he says the medical profession spends too little time on. Most of medical training is about science—physiology, anatomy, pharmacology. Lessons in empathy and personal attention, though they are now included in healthcare education, often end with the close of a humanities elective. But empathy needs to be reinforced, Hojat says; it fades over time. And he argues that it should be part of continuing education for healthcare professionals throughout their career.
“So many more schools are trying to put empathy in their teaching, which tells us maybe we didn’t get it right before,” says Shifrin. “We need to maybe not teach our students to divorce themselves from their humanness. Human connection is essential.”
Header: Med student Anji R. and mentors Mike S. and Mary Anne S. are introduced during a visit to Philadelphia’s Magic Gardens. Photo: Jonas Denzel and Christian Hays